Single Tooth Implants: More Than Meets the Eye
Going From Good to Great: The Role of the Restorative Dentist
Replacement of one missing tooth with a single-tooth implant has become a predictable treatment for our patients. The workflow of the planning, surgery, and restoration, however, has been inconsistent. Many restorative dentists delegate surgeons to make all or most treatment planning decisions. Some surgeons skip important steps, such as 3-D planning, and the use of accurate surgical guides. Some restorative dentists attend weekend courses and learn to surgically place implants, focusing on the so-called 'easy cases,' yet winding up with sub-optimal results.
A better approach to go from good to great with single-tooth implant treatment revolves around teamwork, communication, and a respect for the tissues that have been lost and how to address them. Old school tailors said 'measure twice, cut once.' Sage words that also apply to implant dentistry. Let's look at the following patient's case as a restorative dentist and sharpen our focus and agency to optimize our results.
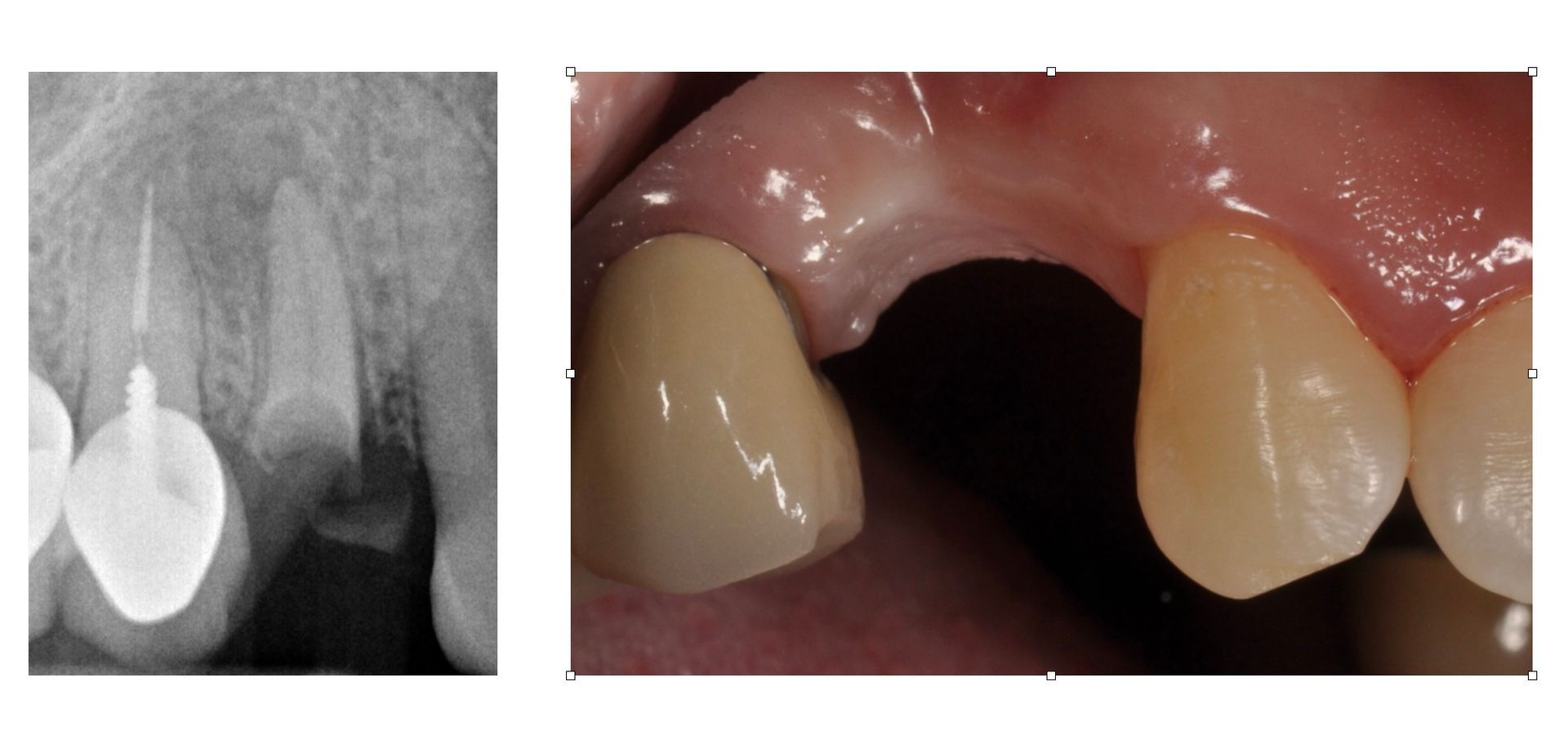
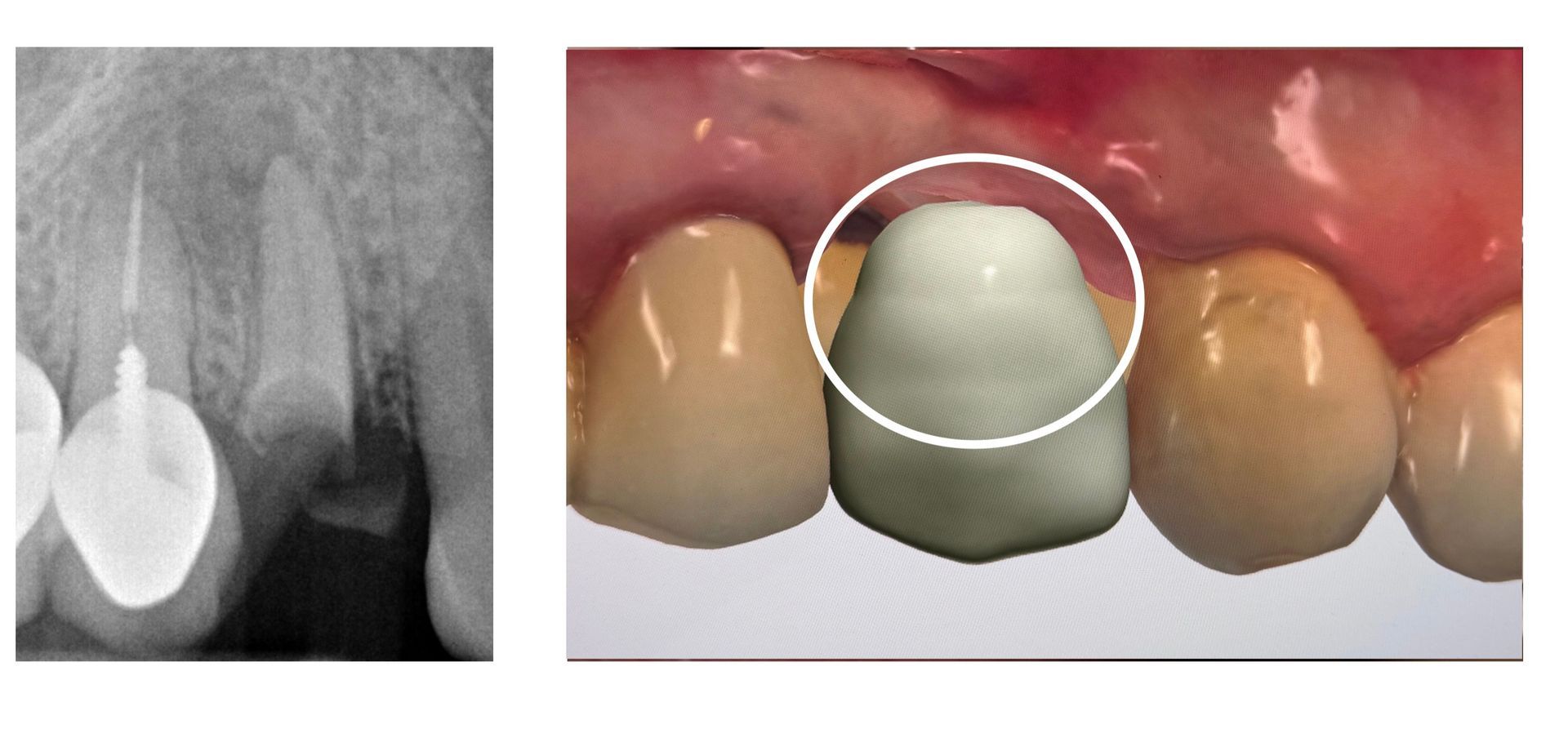
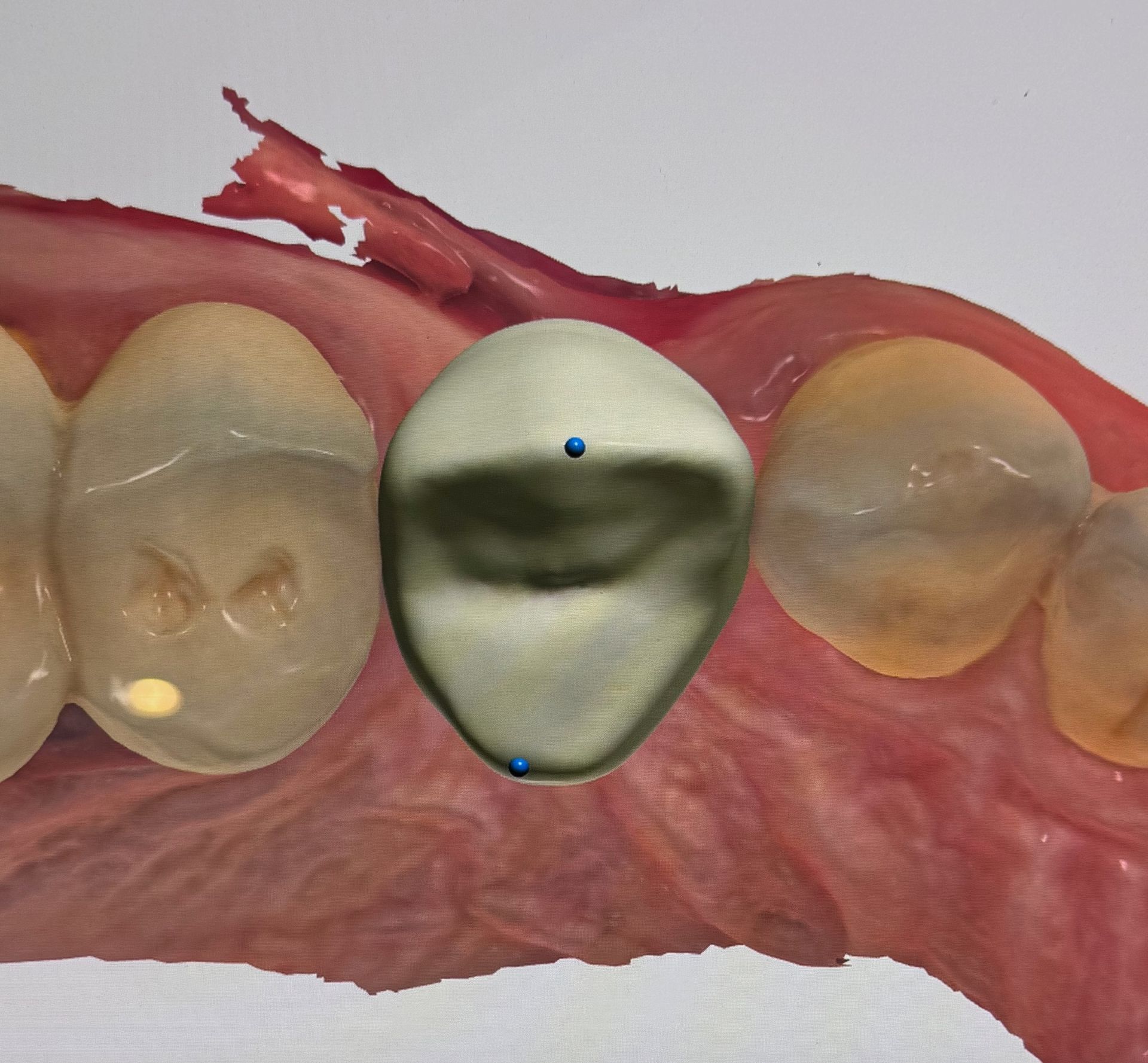
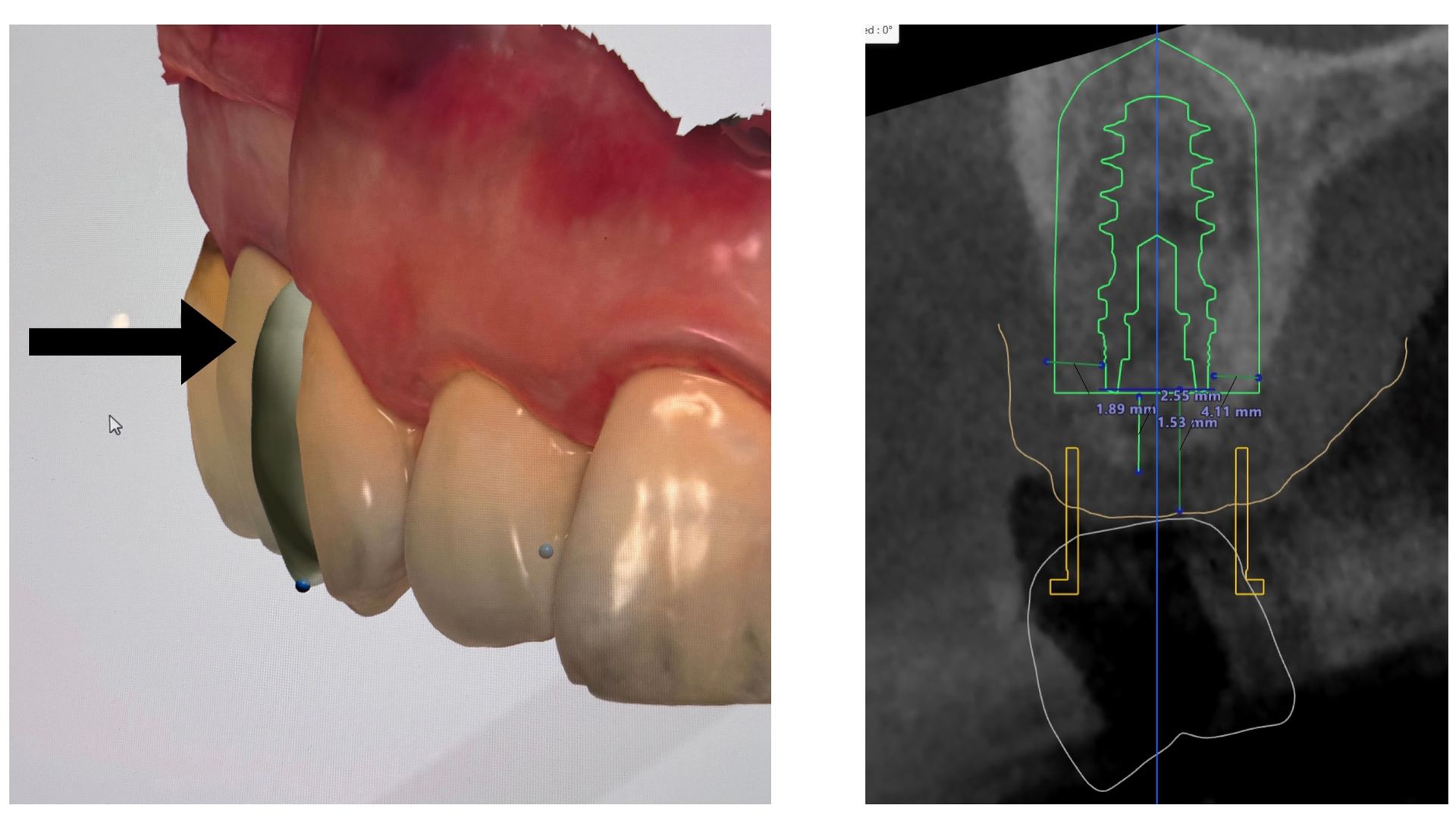
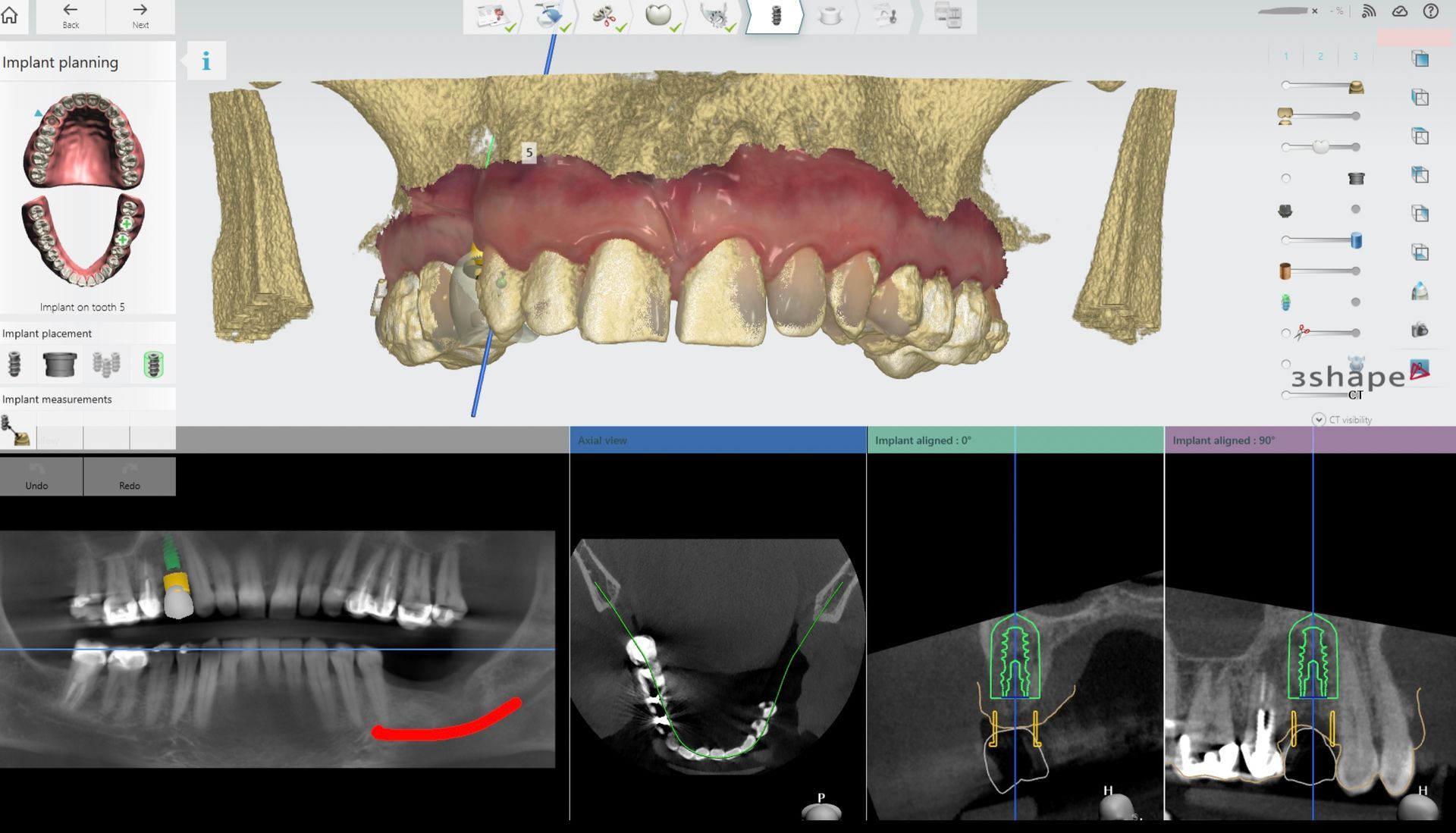
The patient had tooth #5 extracted. What are the next steps? What tissues have been lost? Who on the team does what? First, we combine the CBCT and iOs scan and merge them in 3Shape Implant studio. Combining our study with clinical photos, we can virtually place a Pontic and plan the implant around it. We also notice that tissue and bone are missing. We are not just replacing a missing tooth. We are replacing missing bone and tissue. Options include bone grafting at time of placement, along with an anatomic provisional crown that respects and encourages soft tissue growth. For this patient, the plan has just started. Tune in and join the discussion on this 'simple' case as we move forward to go from good to great in restorative implant dentistry.
Restoratively-driven implant dentistry means Restorative Dentist-driven implant dentistry. Scan and plan.